Antimicrobial activity
Using the agar well diffusion assay, the newly synthesized coumarin derivatives, were estimated for their antimicrobial activity towards S. aureus (ATCC 6538), E. coli (ATCC 25933), C. albicans (ATCC 1023) besides A. niger (NRRL-A326)35. It has been found that the newly synthesized coumarin derivatives exhibited diverse activities in relation to the test microbe (Table 1, Fig. s1). Compounds 4f and 9 had considerable antimicrobial activities against all test microbes with inhibition values of 16 and 16Â mm against S. aureus, 15 and 9Â mm against E. coli, 18 and 17Â mm against C. albicans, and 15 and 19Â mm against A. niger. It has been also found that compounds 4d, 4e, 6a, and 7 had moderate activities against S. aureus with inhibition values of 13, 10, 14, and 12Â mm (respectively), whereas the other compounds exhibited low or no activities against the same test microbe. For E. coli, compounds 4b, 5b and 6b showed low activities with inhibition values of 7, 8 and 7Â mm (respectively) and the other compounds showed negative results. On the other hand, compound 4d had high activity with C. albicans (18Â mm) but compounds 4e and 6a exhibited moderate activities (10 and 14Â mm, respectively) whereas the other compounds showed low or no activities. For A. niger, compounds 4b, 4c, 4d, 4e, 5a, 6a, and 6b had moderate activities (12, 13, 13, 12, 12, 14, and 12Â mm, respectively), whereas the other compounds had low activities.
Further works including minimum inhibition concentration (MIC) and minimum bactericidal concentration (MBC) had been done for the compounds that had comparatively high antimicrobial activates, 4d, 4e, 4f, 6a and 9 (Table 2, Fig. s2)35,36.
The data from Table 2 showed that, compound 9 exhibited the lowest MIC and MBC values for all test microbes with (4.88 and 9.76 µg/mL for S. aureus), (78.13 and 312.5 µg/mL for E. coli), (9.77 and 78.13 µg/mL for C. albicans), and (39.06 and 76.7 µg/mL for MRSA). Additionally, compounds 4f, 6a, 4d, and 4e showed remarkable promising MIC values 9.77, 9.77, 19.53, and 39.06 µg/mL (respectively) and MBC values 39.06, 78.13, 78.13, and 39.06 mL (respectively) against S. aureus. They also showed higher MIC and MBC values against the remained tested microbes. With respect to neomycin, compound 9 was about 4-fold more potent against S. aureus, followed by compound 4f and 6a (about 2-fold more potent). For E. coli compound 9 was less active than neomycin (2-fold lower). In case of C. albicans, both compounds 9 and 4f were more potent than neomycin (4-fold and 2-fold, respectively, while compound 4e was equipotent with neomycin. Out of the selected five compounds MIC study against MRSA, compound 9 was equipotent with neomycin.
Considering the structureâactivity relationship after antimicrobial analysis, compounds 4f, 6a, and 9 showed the antimicrobial activity of the sulfonamide -containing coumarin and the presence of di-coumarin37. Interestingly, active compound 9 may confirm that the presence of two coumarin rings has a high antimicrobial effect against most of the microorganisms studied, consistent with what was previously reported37.
Inhibition of biofilm formation
Microorganisms that can produce biofilms are known to be one of the major factors contributing to antibiotic resistance. Therefore, many experiments have been conducted to overcome these serious problems by searching for new drugs that can prevent biofilm formation38. S. aureus is one of the most frequent causes of biofilm-associated clinical infections. The increasing emergence of methicillin-resistant S. aureus (MRSA), antibiotic resistance, and biofilm-forming capacity contribute to S. aureus being the most commonly identified pathogen in both healthcare and community settings. Additionally, the ability to acquire novel antibiotic resistance mechanisms makes MRSA a major global health threat24,39,40.
Coumarin and its derivatives have attracted the attention of many microbiologists due to their antimicrobial effectiveness41,42. There are also further studies on the effectiveness of coumarin as an inhibitor of biofilm formation20,43. A recent study has proven that 3-hyrdroxy-coumarin, a marine bacterium-derived compound, showed antibiofilm formation44. So, the inhibition of biofilm formation was performed for the five most active compounds 4d, 4e, 4f, 6a, and 9 using neomycin as a reference control compound. Table 3 and Fig. s3 explained the ability of the most active compounds with potent antibiofilm formation expressed as IC50 values. It was found that, compound 9 exhibited the best antibiofilm activities against S. aureus, E. coli, and MRSA with IC50 values of 60, 133.32, and 19.67 µg/mL, respectively in comparison to neomycin (IC50â=â19.67, 79.289, and 39.34 µg/mL, respectively). For the other compounds, it has been reported that compounds 4d and 6a had considerably acceptable results with S. aureus (IC50 of 185.51 and 355.52 µg/mL, respectively). The other compounds had appreciable IC50 values against the same test microbe. For E. coli, compounds 4d and 4e showed noticeable IC50 values 321.25 and 345.40 µg/mL (respectively). All the other compounds (4d, 4e, 4f and 6a) when tested as antibiofilm formation by MRSA, compound 4e and 6a showed promising results (IC50: 85.02 and 40.73 µg/mL, respectively) in respect to neomycin. Out of the five selected compounds for inhibition of biofilm formation, compound 9 was the potent one and showing antibiofilm activity against MRSA (about twofold more potent) and about fivefold and threefold lower against S. aureus, E. coli, respectively.
Effect of compounds on nitric oxide levels in LPS-stimulated RAW 264.7 macrophages
Coumarins represent an important family of oxygen-containing heterocycles, widely distributed in nature45,46. Coumarin and its derivatives exhibited a broad range of biological and pharmacological activities47. A previous study indicated that imperatorin (a coumarin derivative) has an anti-inflammatory effect in lipopolysaccharide-stimulated mouse macrophages (RAW264.7) in an in-vitro model of edema, as it inhibits the protein expression of nitric oxide synthase (NOS) and a cyclooxygenase-2 (COX-2)48. The effect of the active compounds (4d, 4f, 6a, and 9) on levels of Nitric Oxide (Fig. 2A) in LPS-stimulated RAW 264.7 cells was investigated according to the method of Elshahid et al.49. All the cells were treated with the studied compounds along with LPS or LPS alone for 24 h. To determine the level of NO production, the released of nitrite into the culture medium was measured using Griess reagent. As a result, LPS alone markedly induced NO production compared with that generated by the control. However, pretreatment with the studied compounds affected NO levels that significantly produced in LPS-stimulated RAW 264.7 cells as shown in Fig. 2A. Moreover, compounds (4d) induce marked inhibition on NO production by (70%) as compared to LPS (Table 4).
(A) Effects of the studied compounds on the production of nitric oxide (NO) in LPS-stimulated RAW264.7 macrophages. Cells were treated with the studied compounds at concentration 100 µg/mL plus LPS (1 μg/mL) or LPS alone for 24 h. Sulindac (NSAID) was used as a positive control. (B) Cytotoxic effect of the studied compounds and Sulindac on Raw-264.7 macrophages at concentrations (100 μg/mL). Values are expressed as the meansâ±âSD (nâ=â3) pâ<â0.0001 (versus LPS alone, 2A).
In a parallel experiment, to examine the cytotoxicity of the studied compounds on RAW 264.7 cells, the cells were treated with each compound for 24Â h in the presence or absence of LPS, and the cytotoxic potential was measured by the MTT assay50.
The results showed that compound (4d) was the least cytotoxic compound (â 20% cytotoxicity) indicating high cell viability. Meanwhile, compound (4f) and Sulindac (positive control) showed higher cytotoxic effect as indicated by the MTT reduction assay (Fig. 2B). These results clearly indicate that the anti-inflammatory activity of 4d in LPS-stimulated RAW 264.7 macrophages was not due to direct cell death. Accumulating evidence indicates that NO is a critical mediators of inflammation51,52. NO plays a pivotal role in many body functions; however, its overproduction, particularly in macrophages, can lead to cytotoxicity, inflammation, and autoimmune disorders51,52. Our data are in agreement with several in-vitro studies performed with LPS-stimulated RAW264.7 cells, which showed that coumarin and its derivatives have shown a therapeutic effect against edema, eliminating proteins and fluid from injured tissue by activating mechanisms such as phagocytosis, enzyme release, and proteolysis48,53,54.
Experimental part
Chemistry
All reagents and solvents were of commercial grade. Coumarin (Sigma-Aldrich Chemie GmeH, Taufkirchen, Germany). Melting points of the synthesized coumarins were measured on the digital melting point apparatus (Electro thermal 9100, Electro thermal Engineering Ltd., serial No. 8694, Rochford, United Kingdom) and are uncorrected. A Bruker Avance spectrometer (Bruker, Germany) was used to measure the 1H and 13C NMR spectra of new coumarins at 500 and 125 MHz, respectively. Elemental analyses were carried out on a PerkinâElmer 2400 analyzer (USA) and were found withinâ±â0.4% of the theoretical values. TMS was used as the internal standard and hydrogen coupling patterns are described as (s) singlet, (d) doublet, (t) triplet, (q) quartet and (m) multiple. Chemical shifts were defined as parts per million (ppm) relative to the solvent peak.
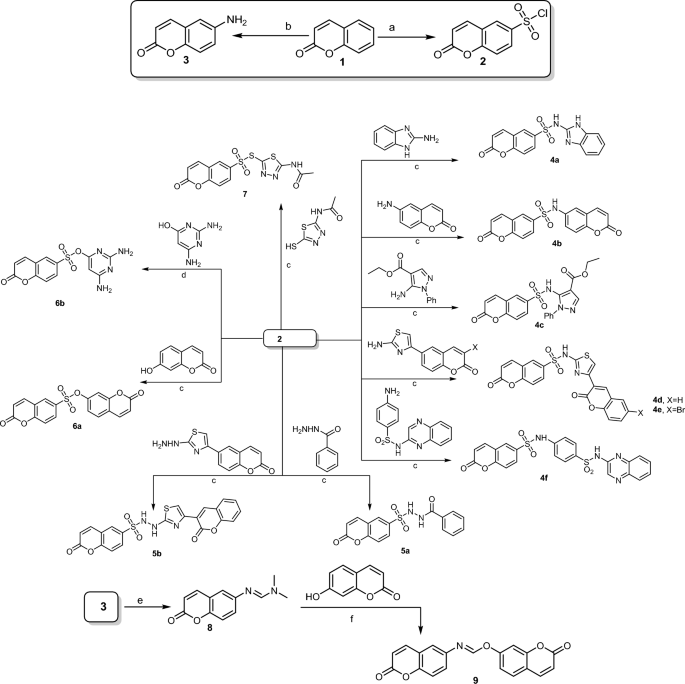
General Procedure for the preparation of coumarin sulfonamide derivatives 4a-f. An equal proportion of coumarin-6-sulfonyl chloride and applicable amino-compounds (10Â mmol) in absolute ethanol (10Â mL) was refluxed under stirring for 5â30Â min. The precipitate formed on hot was collected by filtration and recrystallized from the proper solvent.
N-(1H-benzo[d]imidazol-2-yl)-2-oxo-2H-chromene-6-sulfonamide (4a). Recrystallized from ethanol\DMF as colorless crystals; MP. 295â7 °C; yield: 0.19 g, 55%; 1H NMR (500 MHz, DMSO-d6) δ 12.48 (s, 1H), 8.45 (s, 1H), 8.08 (t, Jâ=â7.5 Hz, 1H), 7.95 (s, 1H), 7.77 (d, Jâ=â8.3 Hz, 1H), 7.45â7.06 (m, 4H), 6.43 (t, Jâ=â8.3 Hz, 1H), 6.14 (s, 1H). Analysis Calc. for C16H11N3O4S (341.34): C, 56.30; H, 3.25; N, 12.31; S, 9.39; Found: C, 56.41; H, 3.33; N, 12.44; S, 9.44.
2-Oxo-N-(2-oxo-2H-chromen-6-yl)-2H-chromene-6-sulfonamide (4b). Recrystallized from ethanol-DMF (5:1) as faint brown crystals; MP. 203â5 °C; yield: 0.30 g, 80%; 1H NMR (500 MHz, DMSO- d6) δ 10.56 (s, 1H), 8.12 (ddd, Jâ=â12.1, 15.3, 7.3 Hz, 1H), 8.06â7.91 (m, 1H), 7.90â7.83 (m, 1H), 7.76 (dd, Jâ=â11.0, 8.2 Hz, 1H), 7.59 (d, Jâ=â10.9 Hz, 1H), 7.50 (dt, Jâ=â10.2, 11.7 Hz, 1H), 7.41 (t, Jâ=â9.7 Hz, 1H), 7.35â7.18 (m, 1H), 6.56 (td, Jâ=â9.8, 6.1 Hz, 1H), 6.46 (ddd, Jâ=â10.7, 9.4, 5.9 Hz, 1H). Analysis Calc. for C18H11NO6S (369.35): C, 58.54; H, 3.00; N, 3.79; S, 8.68; Found: C, 58.45; H, 2.98; N, 3.85; S, 8.73.
Ethyl 5-((2-oxo-2H-chromene)-6-sulfonamido)-1-phenyl-1H-pyrazole-4-carboxylate (4c). Recrystallized from ethanol-DMF (5:1) as colorless crystals; MP. 220â2 °C; yield: 0.29 g, 65%; 1H NMR (500 MHz, DMSO- d6) δ 9.92 (dd, Jâ=â11.7, 9.9 Hz, 1H), 9.61 (s, 1H), 8.28â8.16 (m, 1H), 8.09 (d, Jâ=â12.1 Hz, 1H), 7.95 (dd, Jâ=â2.4, 2.8 Hz, 1H), 7.85 (s, 1H), 7.82â7.71 (m, 1H), 7.68â7.28 (m, 4H), 6.55 (t, Jâ=â8.0 Hz, 1H), 3.34 (q, Jâ=â7.8.0 Hz, 2H), 1.01 (t, Jâ=â6.7 Hz, 3H). Analysis Calc. for C21H17N3O6S (439.44): C, 57.40; H, 3.90; N, 9.56; S, 7.30; Found: C, 57.32; H, 3.98; N, 9.66; S, 7.22.
2-Oxo-N-(2-(2-oxo-2H-chromen-3-yl)thiazol-4-yl)-2H-chromene-6-sulfonamide (4d). Recrystallized from ethanol-DMF (5:1) as green crystals; MP. 260â2 °C; yield: 0.41 g, 90%; 1H NMR (500 MHz, DMSO- d6) δ 8.48 (s, 1H), 8.09 (d, Jâ=â9.5 Hz, 1H), 7.95 (s, 1H), 7.78 (d, Jâ=â9.0 Hz, 1H), 7.73 (d, Jâ=â7.6 Hz, 1H), 7.62 (t, Jâ=â7.7 Hz, 1H), 7.51 (s, 1H), 7.42 (d, Jâ=â8.3 Hz, 1H), 7.37 (t, Jâ=â7.5 Hz, 1H), 7.32 (d, Jâ=â8.5 Hz, 1H), 6.46 (2 s, 2H); 13C NMR (126 MHz, DMSO- d6) δ 169.8, 160.4, 158.7, 154.0, 153.0, 144.8, 144.5, 140.3, 133.2, 129.8, 129.4, 126.0, 125.6, 118.9, 118.4, 116.9, 116.5, 116.4, 109.1. Analysis Calc. for C21H12N2O6S2 (452.46): C, 55.75; H, 2.67; N, 6.19; S, 14.17; Found: C, 55.69; H, 2.77; N, 6.25; S, 14.22.
N-(2-(6-Bromo-2-oxo-2H-chromen-3-yl)thiazol-4-yl)-2-oxo-2H-chromene-6-sulfonamide (4e). Recrystallized from ethanol-DMF (5:1) as crystals; MP. 250â2 °C; yield: 0.43 g, 80%; 1H NMR (500 MHz, DMSO- d6) δ 8.39 (s, 1H), 8.12 (d, Jâ=â9.6 Hz, 1H), 8.04 (d, Jâ=â2.0 Hz, 2H), 7.95 (d, Jâ=â1.6 Hz, 1H), 7.77 (dd, Jâ=â8.5, 1.6 Hz, 1H), 7.70 (dd, Jâ=â8.7, 2.1 Hz, 1H), 7.50 (s, 1H), 7.37 (t, Jâ=â10.7 Hz, 1H), 7.31 (d, Jâ=â8.5 Hz, 1H), 6.51 (d, Jâ=â9.5 Hz, 1H). Analysis Calc. for C21H11BrN2O6S2 (531.35): C, 47.47; H, 2.09; Br, 15.04; N, 5.27; S, 12.07; Found: C, 47.51; H, 2.21; Br, 14.99; N, 5.33; S, 11.98.
2-Oxo-N-(4-(N-(quinoxalin-2-yl)sulfamoyl)phenyl)-2H-chromene-6-sulfonamide (4f) Recrystallized from ethanol-DMF (5:1) as colorless crystals; MP. 203â5 °C; yield: 0.28 g, 55%; 1H NMR (500 MHz, DMSO- d6) δ 12.84 (s, 2H), 7.92 (d, Jâ=â8 Hz, 7H), 7.63 (s, 2H), 7.27 (s, 2H), 6.78 (d, Jâ=â9.6 Hz, 3H). 13C NMR (126 MHz, DMSO- d6) δ 169.5, 167.1, 141.9, 135.5, 135.3, 131.9, 127.9, 127.0, 125.1, 124.1, 109.0; Analysis Calc. for C23H16N4O6S2 (508.05): C, 54.32; H, 3.17; N, 11.02; S, 12.61; Found: C, 54.35; H, 3.22; N, 12.43; S, 12.51.
General Procedure for the preparation of coumarin sulfonohydrazide derivatives 5a and 5b. These compounds were prepared as described for 4 from 2 (10Â mmol) and benzohydrazide or 6-bromo-3-(2-hydrazinylthiazol-4-yl)-2H-chromen-2-one (10Â mmol).
N‘-benzoyl-2-oxo-2H-chromene-6-sulfonohydrazide (5a). Recrystallized from ethanol-DMF (5:1) as colorless crystals; MP. 235â7 °C; yield: 0.17 g, 50%; 1H NMR (500 MHz, DMSO- d6) δ 10.72 (s, 1H), 10.22 (s, 1H), 8.29â8.13 (m, 2H), 7.91 (dd, Jâ=â9.4, 11.1 Hz, 2H), 7.65 (s, 2H), 7.49 (d, Jâ=â8.8 Hz, 2H), 7.39 (s, 1H), 6.59 (d, Jâ=â8.3 Hz, 1H). Analysis Calc. for C16H12N2O5S (344.34): C, 55.81; H, 3.51; N, 8.14; S, 9.31; Found: C, 55.78; H, 3.65; N, 8.22; S, 9.46.
2-Oxo-N‘-(2-(2-oxo-2H-chromen-3-yl)thiazol-4-yl)-2H-chromene-6-sulfonohydrazide (5b). Recrystallized from ethanol-DMF (5:1) as brown crystals; MP. 250â2 °C; yield: 0.42 g, 90%; 1H NMR (500 MHz, DMSO- d6) δ 9.68 (s, 1H), 9.59 (s, 1H), 8.31 (d, Jâ=â8.5 Hz, 2H), 8.19â8.05 (m, 2H), 7.98â7.88 (m, 2H), 7.73 (t, Jâ=â8.8 Hz, 2H), 7.54â7.20 (m, 2H), 6.47 (d, Jâ=â9.5 Hz, 1H). Analysis Calc. for C21H12BrN3O6S2 (546.37): C, 46.16; H, 2.21; Br, 14.62; N, 7.69; S, 11.74. Found: C, 46.10; H, 2.30; Br, 14.72; N, 7.80; S, 11.82.
Synthesis of 2-oxo-2H-chromen-7-yl 2-oxo-2H-chromene-6-sulfonate (6a). This compound was prepared as described for 4a from 2 (10 mmol) and 7-hydroxy coumarin (10 mmol). The product (6a) recrystallized from ethanol-DMF (5:1) as yellow crystals; MP. 259â61 °C; yield: 0.22 g, 60%; 1H NMR (500 MHz, DMSO- d6) δ 8.74 (s, 1H), 8.43 (d, Jâ=â8.7 Hz, 2H), 8.17 (d, Jâ=â9.3 Hz, 1H), 8.00 (d, Jâ=â8.4 Hz, 1H), 7.75 (d, Jâ=â8.4 Hz, 1H), 7.56 (d, Jâ=â9.5 Hz, 2H), 6.63 (d, Jâ=â7.8 Hz, 2H); 13C NMR (126 MHz, DMSO- d6) δ 159.4, 157.18, . Analysis Calc. for C18H10O7S (370.33): C, 58.38; H, 2.72; S, 8.66; Found: C, 58.42; H, 2.65; S, 8.74.
2,6-Diaminopyrimidin-4-yl 2-oxo-2H-chromene -6-sulfonate (6b). To a solution of 2,6-diaminopyrimidin-4-ol (10 mmol) in acetone containing (10 mmol) of K2CO3 was added compound 2 (10 mmol). The reaction mixture was stirring under heat (70â80 °C) for 4 h. The crude product was obtained upon filtration. Recrystallized from ethanol\DMF (5:1) as yellow crystals; MP. 255â7 °C; yield: 0.18 g, 55%; 1H NMR (500 MHz, DMSO- d6) δ 8.17 (d, Jâ=â9.5 Hz, 1H), 7.78 (d, Jâ=â8.1 Hz, 1H), 7.43 (s, 2H), 7.31 (t, Jâ=â7.7 Hz, 1H), 6.48 (d, Jâ=â9.5 Hz, 1H), 4.94 (s, 1H), 2.46 (s, 2H). Analysis Calc. for C13H10N4O5S (334.31): C, 46.71; H, 3.02; N, 16.76; S, 9.59; Found: C, 46.76; H, 3.12; N, 16.89; S, 9.60.
Synthesis of S-(5-acetamido-1,3,4-thiadiazol-2-yl) 2-oxo-2H-chromene-6-sulfonothioate (7). This compound was prepared as described for 4a from 2 (10 mmol) and N-(5-mercapto-1,3,4-thiadiazol-2-yl)acetamide (10 mmol). The product recrystallized from ethanol-DMF (5:1) as crystals; MP. 260â2 °C; yield: 0.27 g, 70%; 1H NMR (500 MHz, DMSO-d6) δ 11.52 (s, 1H), 8.53 (s, 1H), 7.82â7.66 (m, 1H), 7.58 (s, 1H), 6.54 (d, Jâ=â8.6 Hz, 1H), 6.05 (s, 1H), 2.39 (s, 3H). Analysis Calc. for C13H9N3O5S3 (383.41): C, 40.72; H, 2.37; N, 10.96; S, 25.09; Found: C, 40.69; H, 2.40; N, 11.01; S, 24.98.
Synthesis of (E)-N,N-Dimethyl-N‘-(2-oxo-2H-chromen-6-yl)formimidamide (8). N,N-Dimethylformamide dimethyl acetal (10 mmol) was added to 6-aminocoumarin (10 mmol) in xylene (2 mL). The reaction mixture was heated at reflux for (3 h) then left to cool. The brown crystals formed after cooling were collected by scratch. Recrystallized from acetone as honey crystals; MP. 180 °C; yield: 0.13 g, 60%; 1H NMR (500 MHz, CDCl3) δ 7.72â7.50 (m, 2H), 7.29â7.08 (m, 2H), 7.03 (s, 1H), 6.43â6.30 (m, 1H), 3.08 (d, Jâ=â8.8 Hz, 6H). Analysis Calc. for C12H12N2O2 (216.24): C, 66.65; H, 5.59; N, 12.96; Found: C, 66.56; H, 5.64; N, 13.00.
Synthesis of 2-oxo-2H-chromen-7-yl (E)-N-(2-oxo-2H-chromen-6-yl) formimidate (9). Compound 8 (10 mmol) and 7-hydroxy coumarin (10 mmol) in absolute ethanol (10 mL) containing (0.5 mL) of glacial acetic acid was heated under reflux for 2 h. The crude product was collected and recrystallized from acetone as brown crystals; MP. 108â10 °C; yield: 0.2 g, 60%; 1H NMR (500 MHz, CDCl3) δ 8.71 (s, 1H), 8.17 (d, Jâ=â9.3 Hz, 1H), 7.60â7.54 (m, 1H), 7.44 (tdd, Jâ=â9.2, 5.8, 3.0 Hz, 1H), 7.36â7.30 (m, 1H), 7.27â7.24 (m, 1H), 7.20â7.16 (m, 1H), 7.13 (d, Jâ=â8.8 Hz, 1H), 6.90â6.83 (m, 1H), 6.74â6.69 (m, 1H), 6.40â6.34 (m, 1H); 13C NMR (126 MHz, CDCl3) δ 176.7, 161.4, 152.3, 147.9, 143.4, 138.4, 136.2, 127.8, 121.8, 119.4, 119.7, 117.9, 117.5, 116.8, 111.7, 110.2; Analysis Calc. for C19H11NO5 (333.30): C, 68.47; H, 3.33; N, 4.20; Found: C, 68.32; H, 3.21; N, 4.44.
Biological assays
Antimicrobial assay
The antimicrobial activity of the synthesized compounds were assessed against Staphylococcus aureus ATCC 6538-P as Gram positive bacterium, Escherichia coli ATCC 25933 as Gram negative bacterium, Candida albicans ATCC 10231 as yeast as well as the filamentous fungal test microbe Aspergillus niger NRRL-A326 by the agar well diffusion method35. Bacterial and yeast test microbes were inoculated on nutrient agar medium plates seeded with 0.1 mL of 105â106 cells/mL whereas the fungal test strain was cultivated on plates having potato dextrose agar medium that seeded by 0.1 mL (106 cells/mL) of the fungal inoculum. 5 mg of each sample was dissolved in 2 mL of DMSO. 100 µl from each sample were distributed in holes developed in each inoculated plate. Then plates were kept at 4 °C for more than 2 h to allow extreme dispersion. The plates were then kept at 37 °C overnight for bacteria and yeast and kept at 30 °C for 2 days for the fungus in vertical location to permit maximum microbial growth. Neomycin was used as reference drug for Gram-positive and Gram-negative bacteria as well as yeast. Cyclohexamide was used as reference drug for fungi (A. niger). The clear zone diameters expressed in millimeter (mm) were used to differentiate the antimicrobial activity of tested compounds. The experiment was carried out twice and their mean were considered.
Evaluation of minimum inhibitory concentration (MIC) and Minimum bactericidal Methicillin Resistant S. aureus concentration (MBC)
MIC was performed using S. aureus ATCC 6538, Gram-positive bacterium, and E. coli ATCC 25922, Gram-negative bacterium, Candida albicans ATCC 10231 as yeast, and Methicillin Resistant S. aureus (MRSA) as tested microbes that are grown on a Mueller Hinton medium. Test microbes were cultivated in 100 mL bottles with each test at 35 °C for 24 h. Cells were obtained by centrifugation (4000 rpm) under a sterile condition at 4 °C for 15 min. The cells were washed using sterile saline until the supernatant was clear. Cells with an optical density of 0.5 to 1 (at 550 nm) giving an actual number of colony-forming units of 5âÃâ106 cfu/mL were obtained. Resazurin solution was prepared by dissolving 270 mg tablet in 40 mL of sterile distilled water. Then, 96-well sterile microplates were prepared. Then, 50μL of test material in DMSO was pipetted into the first row of the plate. To all other wells, 50μL of broth medium was added. Two-fold serial dilutions were performed. Then, 10μL of resazurin indicator solution was added, 10μL of bacterial suspension was added to each well. The plates were prepared in duplicate and placed in an incubator set at 37 °C for 18â24 h. Any colour changes from purple to pink or colourless were recorded as positive. The lowest concentration at which colour change occurred was taken as the MIC value. MBC has been performed by streaking of the two concentrations higher than MIC and the plates exhibiting no growth were considered as MBC35,36. Neomycine has been used as positive control55.
Inhibition of biofilm formation (crystal violet method)
Bacterial strains were incubated in test tubes with TSB (5 mL) containing 2% w/v glucose at 37 °C for 24 h. After that, the bacterial suspensions were diluted to achieve turbidity equivalent to a 0.5 McFarland standard. The diluted suspension (2.5μL) was added to each well of a single cell culture polystyrene sterile, flat-bottom 96-well plate filled with TSB (200μL) with 2% w/v glucose. Sub-MIC concentration values of compounds 4d, 4e, 4f, 6a, and 9 were directly added to the wells to reach concentrations ranging from 100 to 0.1 μM to assess BIC50 values that are, the concentration at which the percentage of inhibition of biofilm formation is equal to 50%. Plates were incubated at 37 °C for 24 h. After biofilm growth, the content of each well was removed, wells were washed twice with sterile NaCl 0.9% and stained with 200μL of 0.1% w/v crystal violet solution for 15 min at 37 °C. The excess solution was removed, and the plate was washed twice, using tap water. A volume of 200 μL of ethanol was added to each stained well to solubilize the dye35,38. Neomycine has been used as positive control55. Optical density (O.D.) was read at 600 nm using a microplate reader (GloMax®-Multi Detection System, Milan, Italy). The experiments were run at least in triplicates, and three independent experiments were performed. The percentage of inhibition was calculated through the formula:
$$ \% {\text{ Inhibition}} = \left( {{\text{OD}}\;{\text{growth}} – {\text{OD}}\;{\text{sample}}/{\text{OD}}\;{\text{growth}}\;{\text{control}}} \right) \times {1}00 $$
(1)
Antiâinflammatory assay
Cell culture (seeding and treatment)
The RAW 264.7 macrophage cell line were supplied from ATCC (American type culture collection).The cells were sub-cultured in Roswell Park Memorial Institute’s RPMI 1640 medium49.
Procedure
The following procedures were all completed in a biosafety level II Laminar flow cabinet in a clean environment. RAW 264.7 cells were suspended at concentration of 1âÃâ105 cells per well (in 96 well plates). The cells were then incubated with the test compounds, LPS (lipopolysaccharide, negative control) and Sulindac (positive control drug) according to the method49. After 24 h, the supernatant was gently transferred to new 96-well plates for measuring nitric oxide (NO) while cells were used for cell viability testing using the MTT method. The percentage change in viability was calculated according to the below formula
$$ \left( {\left( {{\text{Reading}}\;{\text{of}}\;{\text{extract}}/{\text{Reading}}\;{\text{of}}\;{\text{negative}}\;{\text{control}}} \right) – {1}} \right) \times {1}00 $$
Nitric oxide assay
The generation of nitric oxide (NO) was measured in the supernatants of cultivated RAW 264.7 cells. With slight modification, the Nitric Oxide (NO) measurement was carried out as described by Eid et al.50 using the Griess reagent. In detail, 50 μl of cell culture media were added to 50 μl of Griess reagent then incubated at room temperature for 15 min before being measured at 540 nm50. A sodium nitrite standard curve was used to calculate the amount of nitrite, as shown in equation:
$$ {\text{Nitric}}\;{\text{Oxide}}\;{\text{inhibition}}\left( \% \right) = \frac{{\left( {{\text{control}} – {\text{Test}}} \right)}}{{ {\text{control}}}} \times {1}00 $$
Statistical analysis
All statistical analysis and IC50 values were calculated using the concentrationâresponse curve fit to the non-linear regression model and One-way ANOVA with Dunnetâs posttest was performed using GraphPad Prism® v7.0 (GraphPad Software Inc., San Diego, CA, USA).